Botox injections combined with an anti-Neausea patch can help advanced metastatic patients with prostate cancer (MCRPC) avoid severe dry mouth and continue the treatment of radiofrequency, proposing early research on June 24th. (SNMMI).
The toxicity of the silent gland is a well-known side effect of some prostate antigen (PSMA) that can be targeted at radio frequency treatment (RLT)-especially alpha-ray-225 (AC-225)-which can lead to unfair, Xerostomia Syndrome, Zhang, MD, PhD, PhD, PhD, PhD, PhD, Phd. at the Yong Loo Lin School of Medicine at Singapore National University.
However, the combination of Botulinum (BTX) toxin (INCOA) and nausea patch (screech) It can offer a double protection approach, both, having created security profiles, could be applied immediately to experienced centers that offer PSMA radio frequency treatment, Zhang and his colleagues wrote.
To investigate the impact of the double approach, the group conducted a preclinical study of early oncology oncology oncology that included 14 patients undergoing one to two cycles of successive treatment with PSMA-targeted radio frequency, lutetium-177 (LU-177) in 6.87 ± 3.14 MBQ per cycle.
Each patient received 16 BTX treatments consisting of 115 to 250 units of ultrasound guided BTX INCOA injections into their parotid glands and between 70 to 80 units in their sub-column glands on the opposite sides of the body, three to four weeks before their AC-225 PSAs. Four patients only treated with BTX, while others received a combination of BTX plus scolamine patch.
Three days before treatment, the nausea patches were applied behind the ears, where they remained up to two hours after treatment.
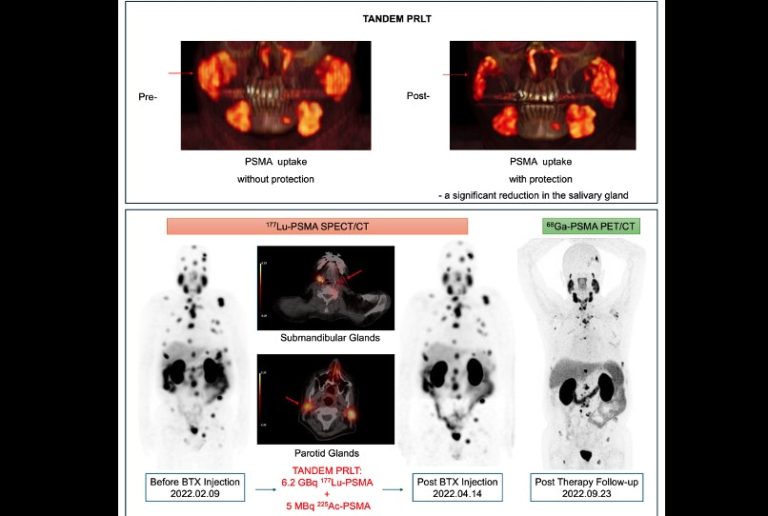
Patients also underwent PSMA PET/CT pre-treatment to confirm the intake of tumor and salivary gland and SPECT/CT after treatment for rehabilitation, according to the group.
Researchers found that the btx mocotetic glands showed an average reduction of 30% (19% to 47%) in the PSMA intake (p <0.001) compared to the opposite parotid gland. They also reported an average reduction of 17% (10-51% range) in PSMA intake in infused hypomanic gambles (p = 0.004) compared to the opposite component glands.
The SPECT/CT images after the injection revealed a remarkable reduction in the recruitment of radiofrequency PSMAs in the BTX -treated glands, with the ratio of parodiac glands shifted from 0.93 to 1.15 and a proportion of subordinates from 1.39 to 2.14, confirmed by protection.
Patients receiving BTX without scolmine did not show a significant difference in the intake between injected and uninvited salivary glands, they said, adding that injections were generally tolerated and, above all, no patients interrupted by PSMA treatment that did not discontinue the patient.
A local infusion -related hematoma appeared in a patient with thrombocytopenia, the group said. Also, a medium dry mouth caused by scorolamine, but lasted 72 hours.
“This study offers a very promising therapeutic strategy to reduce the toxicity of the salivary gland caused by radiation without at stakeing the intake of PSMA tumor,” Zhang said. “The importance of this work lies in the immediate benefit of the patient and to his or her ability to extend the therapeutic utility of PSMA radio therapy, especially with alpha radionucuts such as 225ac.”
The researchers concluded that the combined approach can enhance the quality of life of patients after PSMA radio frequency treatment, especially with alpha radionuclides, although further studies with larger patient groups and longer surveillance periods are justified.