What are the symptoms of varicose veins?
The most recognizable sign of a varicose vein is a varicose, blue or purple vein just below the surface of your skin. Symptoms of varicocele include:
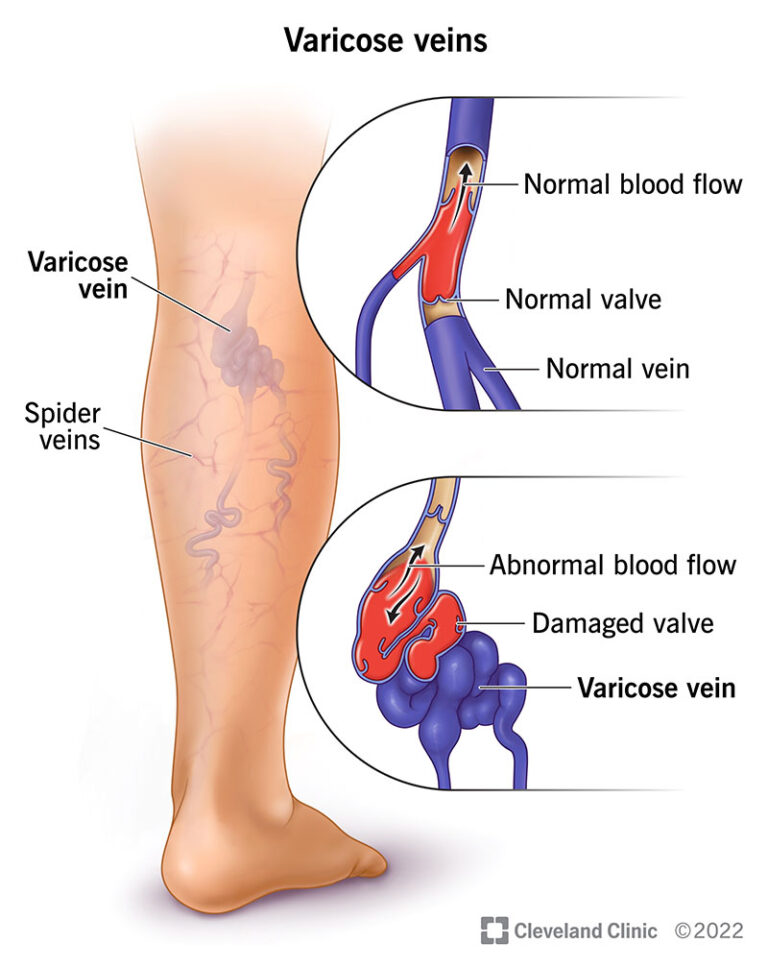
- Varicose veins: Twisted, bulging, rope-like veins are often blue or purple. They appear just below the surface of the skin on your feet, ankles and legs. They can grow in groups. Tiny red or blue lines (spider veins) may appear nearby.
- Heavy legs: The muscles in your legs may feel tired, heavy, or sluggish, especially after physical activity.
- Itching: The area around a varicocele may itch.
- Pain: Legs may be sore, achy or sore, especially behind your knees. You may have muscle cramps.
- Swelling: Your feet, ankles, and legs may swell and throb.
- Skin discolorations and ulcers: Left untreated, varicose veins can cause discoloration of your skin. Severe varicose veins can cause venous ulcers (sores) on your skin.
Where do varicose veins usually appear?
Most of the time, varicose veins develop in the lower half of your body, usually in your calves, ankles and feet. They can also develop in the pelvic area (pelvic congestion syndrome), especially in people who have had children. Hemorrhoids, which form in your rectum, are also varicose veins.
What causes varicose veins?
Varicose veins occur when the walls of your veins weaken. As the blood pressure in your vein increases, the weakened walls allow your vein to enlarge. As your vein stretches, the valves that keep blood moving in one direction in your vein can’t work as they should. Slow blood backs up or pools in your vein, causing your vein to swell, bulge, and twist.
Vein walls and valves can become weak for a number of reasons, including:
- Normal aging.
- Standing for extended periods of time.
- hormones.
- Excess weight.
What are the risk factors for varicose veins?
Anyone can develop varicose veins. Certain factors increase your chances of developing a varicocele, including:
- Age: Due to the aging process, the vein walls and valves do not work as they used to. Veins lose elasticity and harden.
- Hormones: Female hormones can allow the vein walls to stretch. Women who are pregnant, on the pill, or in menopause have a higher risk of varicose veins due to changes in hormone levels.
- Family history: You can inherit this condition if it runs in your family.
- Lifestyle: Prolonged standing or sitting reduces circulation.
- General health: Certain health conditions can increase the pressure in your veins.
- Use of tobacco: People who use tobacco products are more likely to develop varicose veins.
- Weight: Excess weight puts pressure on blood vessels.
What are the serious complications of varicose veins?
Most people do not have complications from varicose veins. But in some people, an untreated varicocele can cause ulcers (open sores), bleeding, inflammation or discoloration of the skin. Severe varicose veins can be a sign of chronic venous insufficiency (CVI). This condition affects the ability of your veins to pump blood to your heart.
If you have varicose veins, you may be more likely to develop blood clots. It is important to tell your healthcare provider about varicose veins so they can evaluate and monitor you for clotting disorders. These include:
- Superficial thrombophlebitis: Blood clots can form inside the varicose veins, causing superficial vein thrombosis or superficial thrombophlebitis. Thrombophlebitis is painful but usually not dangerous. It is also treatable.
- Deep vein thrombosis (DVT): If you have varicose veins, you have a higher risk of deep vein thrombosis, a blood clot in a vein deep in your body.
- Pulmonary embolism: A blood clot in your body (usually from a DVT) can travel into your lung. Pulmonary embolism is a life-threatening condition that requires immediate treatment.