Chronic diseases and systemic diseases are inextricably linked to the health of our mouths. Have about 15 million people in the UK a long -term medical condition that affects them every day.
New investigation It shows the two -way relationship between the oral cavity and various serious conditions such as rheumatoid arthritis, cardiovascular disorders, diabetes mellitus and chronic respiratory diseases.
We need to encourage our patients to adopt a preventive approach to their health and to require better oral health care for those living with chronic diseases. The government must also adopt a preventive approach with improved funding, encouraging interdisciplinary treatment and greater access to preventive care. This will reduce oral pain, illness and further expenses for NHS.
Illness and inflammation of the gums
Gum disease is the body’s response to harmful pathogens in the mouth, activating an immune response that can affect both oral and systematic health. When detected early, it is often controlled. However, the disease that has not been treated can contribute to chronic inflammation, worsening conditions such as arthritis. This emphasizes the urgent need for further research and funding for a better understanding of the relationship between gum disease and inflammatory diseases.
Despite its broad impact, access to early diagnosis and treatment for gum disease remains inconsistent throughout the United Kingdom. Many patients are struggling to secure dental appointments, limiting opportunities for early intervention. Peripheral inequalities in the availability of dental workforce exacerbate this issue – recent evidence shows that the South West has the highest percentage of vacancies for fully qualified dentist at 22%compared to 15% in London. The availability of NHS treatment also varies, with only 60% of the time of dentists available in the care of NHS in the southwest, compared to 77% in northeast and Yorkshire.
Emergency action is required to effectively treat the disease to ensure fair access to dental care. This includes increased government investments in NHS dentistry, expansion of workforce and the strongest educational policies that prioritize the prevention of gum disease. Without these measures, the increasing weight of the gum disease will continue to negatively affect both individual and public health.
Impact on cardiovascular health
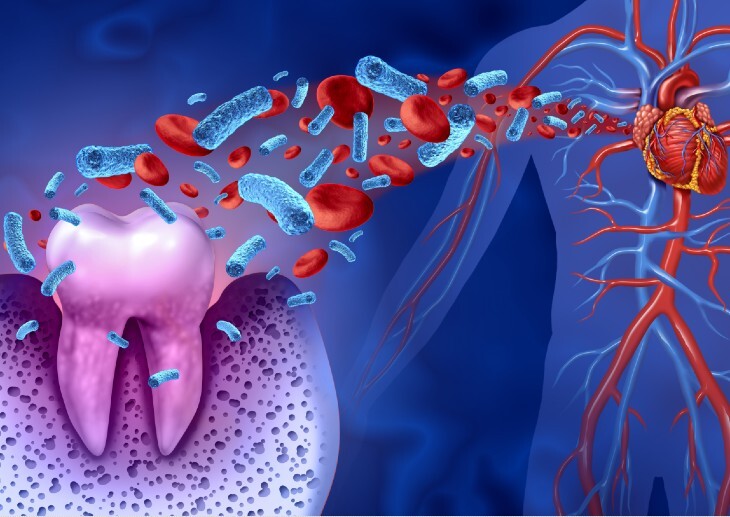
Poor oral health can cause serious problems for heart health. Oral bacteria can spread to the valves of the heart through blood circulation, causing endocarditis.
That is why poor oral care is dangerous for people with pre -existing heart disease. One of the best actions that patients can take home to help their overall health is to prioritize preventive care and take care of their health in their mouths.
We need to encourage patients during the appointments of the doctor and dentists to see their oral health as an inherent part of their general prosperity. One in four (25%) adults Do not brush their teeth regularly twice a dayOne in three (33%) have never surpassed or cleaned. Meanwhile, two in three (66%) adults have a visible plate. These are shocking statistics for the United Kingdom and we need to change our attitude towards the care of our oral health.
Dental visits can catch early signs of oral health problems, facing problems before escalating to develop professional paths to ensure good treatment that is at all.
When patients have potential for heart problems, they should be encouraged to examine their oral health at home. In order for this to work, there must be an interdisciplinary approach and a two -level approach that includes the patient’s doctor and dentist to achieve the best results.
Branches of diabetes
THE The latest data show that nearly 4.6 million people in the UK live with diabetes. In addition, nearly 1.3 million people could live with type two diabetes which are But to be diagnosed. Diabetes can affect the whole body and mouth.
Patients living with and managing diabetes have a higher risk of caries. Excessive sugar in a patient’s blood can lead to more sugar in saliva. More sugar equals more energy to grow and multiply the bacteria. These bacteria produce acid plate that attacks teeth by increasing the risk of caries.
They are common for patients with diabetes, both type 1 and type two to develop dry mouth. Ownership of chronic oral mouth is also a risk factor for tooth wear.
There were projection tests for Diabetes in the past in dental practices. The results of these studies have proven vital to highlighting a potentially non-diagnosed type-2 diabetes. This is an excellent example of professionals who work together to provide better overall care and improve patients’ paths to treatment.
Respiratory and oral diseases
Respiratory and oral diseases are linkedParticularly the flu, asthma, COPD and pneumonia. Due to air streets through the mouth to the lungs, the pathogens have an immediate front and back path through breathing. As a result, “There is a vicious loop with whom lung diseases, oral disorders and disorders in the oral microbiotic constantly get worse‘.
In the treatment of respiratory diseases, oral hygiene should be concern for patients, doctors and dentists to prevent the patient from continuing to be sowing. Our patients need a preventive approach to taking care of their overall health. If they can manage their oral care, we need to provide training and support to equip them to prevent dental disease and thus improve respiratory conditions. Carers should also have this opportunity to learn about oral health care.
This is not just a case of education, but also ensuring that it is widely distributed and available to all who need it. The government and policy -makers should prioritize oral health knowledge to help reduce weight and pressure on NHS.
Conclusion
As clinical research continues to enhance the relationship between oral health and systemic disease, it is clear that good oral health should be recognized as a fundamental part of overall health care. Addressing links between oral and general health requires a multi -scientific approach, ensuring that all health professionals are equipped to discuss and promote preventive care with their patients.
Greater awareness and education are essential – especially for those living with chronic diseases known to have an impact on oral health. Prevention messages should be strengthened at all patient contact points, with medical and dental professionals to preventive patients for these critical links. This responsibility cannot rest exclusively with a profession. It requires a collaborative effort in all sectors of health care to integrate oral routine care.
Currently, under -employment in the NHS dentistry has a significant obstacle to achieving these goals. Treating this deficit, along with increasing access to preventive care, should be a priority if we are to improve the results of patients and reduce the broader health burdens associated with poor oral health. The need for action is urgent – without it, we run the risk of failing those who will benefit more than a more comprehensive and preventive approach to health care
Related articles