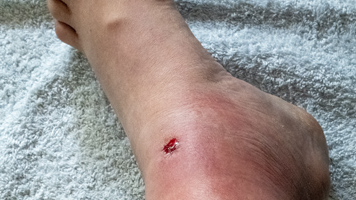
Reasons
Many bacteria can cause cellulitis, an infection in the subcutaneous tissues.
This page focuses on one of the most common causes of cellulite: Streptococcus pyogenes. S. pyogenes also called group A Streptococcus (group A streptococcus bacteria).
Risk factors
Anyone can get cellulite, but certain factors increase a person’s risk.
Breaks into the skin
Disruption of the skin barrier is a risk factor for the development of cellulite:
- Chicken pox and shingles
- Chronic skin conditions (eg eczema)
- Fungal skin infections (eg athlete’s foot)
- Injecting drug use
- Injuries and wounds (eg ulcers)
Medical conditions
- Chronic edema
- Disturbance of the lymphatic drainage of the extremities
- Portliness
- Venous insufficiency
Increased risk of recurrent infections
The following conditions increase a person’s risk for repeated cellulitis infections:
- Disturbance of the lymphatic drainage of the extremities
- Venous insufficiency
- Due to saphenous vein removal for coronary artery bypass grafting
Clinical features
Local signs
Local signs of inflammation are present in most cases of cellulitis:
Systemic symptoms
Systemic symptoms may be present:
These symptoms may be accompanied by lymphangitis and, less commonly, by bacteremia. An elevated white blood cell count may also be present.
Differentiation of other skin infections
Cellulitis affects structures that are deeper than the areas affected by wax or erysipelas.
Diagnosis and control
The diagnosis of cellulitis is usually made clinically.
Routine cultivation is not recommended
For cellulitis, the Infectious Diseases Society of America (IDSA) does not recommend routine culture collection, including
- Biopsies
- Blood
- Skin suctions
- Coatings
When culture is recommended
However, they may be useful when severe systemic features (such as hypotension) are present or atypical pathogens are suspected. For this reason, these procedures are recommended by IDSA for
- Animal bites
- Submersion injuries
- People with an immunocompromised state
Treatment
Never delay starting treatment while waiting for culture results.
Use culture results, when available, to adjust antibiotic therapy.
Antibiotic treatment for non-purulent cellulitis
IDSA recommends treatment with an antibiotic that is active against streptococci. Healthcare providers can choose antibiotics that cover both Staphylococcus aureus and group A streptococcus.
Treatment options
Treat mild cellulitis with oral antibiotics and consider intravenous antibiotics for systemic infections. Group A streptococcus remains susceptible to beta-lactam antibiotics.
Duration of treatment
The recommended treatment duration is 5 days for most cases of cellulite. Cases in which there has been no improvement during this period of time may require a longer duration of treatment.
Another treatment
In addition, the following actions are recommended to reduce the risk of recurrent infection:
- Elevate the affected area
- Management of predisposing factors (eg, edema, underlying skin disorders)
Complications
Complications from cellulitis are uncommon but can include serious infections.
Sometimes: Cellulitis can lead to bacteremia.
Rarely: Cellulite can lead to deep tissue infections, such as
- Infective endocarditis
- Necrotizing soft tissue infections
- Osteomyelitis
- Septic thrombophlebitis
- Suppurative arthritis
Prevention
Reduce the spread of group A strep bacteria with standard infection control practices, including good hand hygiene and respiratory etiquette.
Wound care
Early recognition and management of superficial skin lesions is also key to preventing cellulite. Patients with recurrent cellulitis of the lower extremities should be screened for tinea pedis (athlete’s foot) and treated if present. Traumatic or bite wounds should be cleaned and treated appropriately (eg, antibiotic prophylaxis, surgical debridement if indicated) to prevent secondary infections.